Laying the Foundations of Cuban Revolutionary Healthcare
LATIN AMERICA AND THE CARIBBEAN, 13 Jun 2016
The consciousness of the 3000 doctors who stayed became a material force in the production of Cuban health care.
6 June 2016 – During the first five years of the Cuban revolution half of its 6000 doctors left. But just as professionals were forsaking their homeland for the comforts of Miami, 3000 doctors chose to stay. Why did they remain? More important, with twice as many patients per doctor, how did they face the daunting task of transforming medicine?
Ten years after the revolution, Fidel Castro reflected on the enormity of health care problems that confronted Cuba in January 1959:
The absence of a national public health plan; semi-official and private services that were better than those provided by the government; an orientation toward curative medicine; abandonment of rural and some urban areas; individual medicine; mercantilism; competition between private services; administrative centralization with a public unaware of treatments that could benefit them.
In addition to Fidel’s observations, there was no reliable data on health indicators, an insufficient number of doctors and dentists being graduated, and severe underfunding of the few research facilities that existed. Medical education was theoretical with little hands-on experience and there were too few teaching hospitals.
The principal health care task during the first years of the revolution was creating services. By 1963 the revolutionary government had established 122 rural centers and 42 rural hospitals with 1155 beds, 322 doctors and 49 dentists.
In order to accomplish the primary task, it was necessary to bring cohesion to the disjointed medical system. In January 1960, the revolutionary government created the Ministerio de Salud Pública (MINSAP, Ministry of Public Health) and established Rural Health Services.
Revolutionary changes cannot happen just because laws decree that they will. They require the type of mobilization campaigns that swept Cuba. There were efforts to end unemployment, increase the salary of 350,000 sugar cane workers, implement a pension system, end discrimination in accessing beaches, build 10,000 new classrooms, and send 3000 teachers to rural areas. A new rationing system ensured equitable distribution of food and consumer goods. The literacy campaign was the best known of the mobilization efforts. Within a few years of the revolution, illiteracy was brought down to zero.

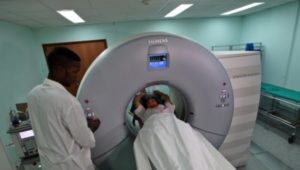
A pregnant woman in Cuba with HIV would be referred to a clinic, like the one above, for specialized care. (photo: Pan American Health Organization)
Medical campaigns were an essential component of this much broader social transformation. In February 1960 the first group of 357 doctors went to rural areas where there had previously been no doctors. Many had to stay in the homes of campesinos. They found people so much in need that initially they could provide only curative, rather than preventive, medicine. Determination for preventive medicine prevailed: By the end of 1960, doctors had given twice as many DPT vaccines as had been provided during all of 1954–59.
The anti-malaria campaign began in 1961. The next year saw the first national campaign to vaccinate against polio, a clean water campaign, gastroenteritis control and a major program to improve staff training.
Medical campaigns in rural Cuba deeply affected those who participated. Dr. José Gilberto Fleites Batista “…will always remember the particular case of a dehydrated little boy. We gave him intravenous infusions because he had diarrhea. I remember that boy well because he would have died of dehydration if we hadn’t been there.”
New Doctors, New Education
The wave of revolutionary fervor sweeping through the island had a particular form in medical school. Batista had responded to protests by closing the University of Havana (including the medical school) in 1957–58. It reopened in 1959 with a new approach.
Inspired by free tuition, those from working class backgrounds were more numerous among new students. Incoming students were required to take classes focusing on rural and tropical medicine as well as preclinical sciences. For the first time, medical school taught biochemistry. Hospital internships were made a prerequisite for graduation. After 1959 social medicine was included in each year’s curriculum.
Student and government involvement was reforming old systems of faculty control of education. That reform took its toll. In August 1960, only 19 professors remained in the medical school — the only one in Cuba. They formed the nucleus of young, competent doctors who took on monumental responsibilities to sustain medical training.
To help in the transition, MINSAP contracted for medical instructors from 26 countries. Most came from Argentina, Mexico, and Ecuador. Others were from Bulgaria, the Soviet Union, Czechoslovakia and Hungary.
To accommodate more students, the number of teaching hospitals increased from 4 to 7 and new medical schools opened in Las Villas and Santiago de Cuba. Students and doctors adjusted to the strenuous demands of the revolution. “No one rested during those years,” Dr. Felipe Cárdenas Gonzáles reminisced. “We worked as hard as we needed to. I did guardia for 24 hours and then I did surgery and then I had to study and write a work-up for new students.”
As Cuban society polarized, students were entering medical school with the expectation that they would be trained, not for personal gain, but according to the needs of society. Renouncing private practice, a popular comment by students was that they would go “wherever the revolution needs me.”
To the Countryside – To the World
Cuba’s medical system interacted with other countries in many ways. As early as April 1961, Cuba signed a cooperation agreement with Czechoslovakia. The next year it sent technicians to Bulgaria to study preventive medicine. East Germany made an agreement in 1964 to send orthopedic supplies.
Cuba also sent doctors abroad. In March 1960, only 15 months after the revolution, an earthquake hit Chile and Cuba sent a few doctors for a brief period. The next year Cuba sent arms to Algerians fighting for independence from France. The boat returned with 76 injured Algerians and 20 child refugees.
A 1963 medical brigade to Algeria had 55 Cubans, including 29 doctors. There were 43 men and 12 women. Details of this mission were not widely known until Hedelberto López Blanch published Secret Stories of Cuban Doctors, a collection of oral histories of Cuban medical workers serving in Africa in the 1960s and 1970s.
One of the doctors going to Algeria was Sara Perelló Perelló, who was 84 years old when interviewed by López. She had just graduated with a specialty in pediatrics. Her mother heard Fidel saying: “There are 4 million more Algerians than Cubans but they have only a third of the doctors we do.”
After her mother told her that she needed to help them, Dr. Perelló went to MINSAP to volunteer. She was worried that her mother had Parkinsons. Her mother responded that Sara’s sister and husband would help her as would the government. “Now the thing to do is go forward and don’t worry about your mother who will be well taken care of.”
Dr. Zoila Italia Suárez would have completed her pediatric specialty; but, due to Batista’s closure of the university, her graduation was delayed until 1960. She went immediately to Granma province for her rural services.
Her recruitment to the Algerian brigade personified the transition from campaigns to end the rural/urban dichotomy within Cuba to medical internationalism. Willingness to leave Havana for rural Cuba easily transferred to a willingness to leave Cuba to help meet medical needs in Africa.
Language was Dr. Italia’s main problem. During treatment she would have one translator for Arabic to French and a second for French to Spanish. When one woman brought in a child but spoke a form of Arabic that the translator not understand, the mother took her hand and put it on her son’s abdomen. Upon feeling a tumor she sent him to the hospital immediately. She learned to diagnose based on where the mother touched the child or if she sneezed or coughed.
The mission taught staff valuable medical experiences. Dr. Italia witnessed “…many sicknesses that were rare or non-existent in Cuba. I saw a lot of tuberculosis, malnutrition, malaria, parasitic diseases and bacterial infections … In Constantina, a military hospital was completely empty because the French doctors had left.”
Ernesto “Che” Guevara left a deep mark on this formative mission. Dr. Italia recalled that “Che visited us when we had only been in Algeria a month. He asked if we were having any difficulties and how we were able to interact with patients without knowing their language. Che only spent a few hours with us; but, we were distributed in various provinces and he went throughout the country.”
The 3000 Who Left
Many Cuban doctors had no desire to go to the provinces, much less to the Algerian desert. Two waves of doctors left. The first accompanied the huge changes in health care delivery during the first couple of years. Many were owners of private clinics, directors of mutualist centers and those with a high income private practice. Others departed with the advent of rural service which would take them to locations lacking in the comforts of Havana. The second wave was provoked by the April 1961 Bay of Pigs invasion and the October 1962 missile crisis.
The literacy, medical and other campaigns that engulfed Cuba’s poor, working, and farming classes were an affront to middle class life styles. It went beyond the disruption of medical school — when Batista closed the university during 1957–58 there was no great exodus of medical faculty. Dr. Ezno Dueñas Gómez suggested, “Many doctors went to Miami not because they were counterrevolutionaries but because they could have so many things in the U.S.”
Pre-1959 attitudes could always predict what a doctor would do once Batista was out. Some who were enthralled by the July 26 Movement but became dismayed once they saw it actually implementing its ideas. Contrariwise, many remained aloof from the struggle, perhaps believing that Cuba could never have a genuine transformation, who threw themselves into it once they saw it happening. The contrast between doctors who stayed and those who left was whether they were enraptured or repulsed by the changes unfolding before their eyes.
Race in the Time of Medical Revolution
African lineage is higher among rural Cubans and those living in the eastern part of the island. The 1959 revolution ushered in the most significant changes in the lives of black Cubans since the abolition of slavery. Calls to serve in rural areas and eastern provinces were synonymous with appeals to fight structural racism.
Pre-revolutionary racism was often open and uncompromising. Dr. Julio López Benítez described “… one hospital that claimed that it was dedicated to religious goals; but it would not accept black patients.”
Dr. Oscar Mena Hector’s family knew racism well. His “…cousin, José Villena, studied medicine but was poor and had to sell tomatoes to buy books. He passed all his courses, but after his last exam, learned that he would not become a doctor because he was black.” At the end of studies there was a tribunal exam and one examining physician would not pass black students. “Two years later, in 1959, he passed his exams and became a doctor.”
The pre-revolutionary period was not without anti-racist efforts within health care. In 1938 the communist-led Transport Workers Union began a mutualist health plan with a clinic for its workers, the Centro Benéfico. After five years it offered the plan to other workers and enrolled 25,000 by 1959. It was the only mutualist clinic which had a large number of nonwhite Cubans and did not practice segregation.
The outpouring of medical teams to poor urban communities, rural areas and the eastern part of the island with coordination by the revolutionary government occurred at the same time that U.S. civil rights demonstrators were being beaten by police and attacked by dogs for demanding the right to sit at “whites only” lunch counters.
Consciousness
The central contradiction facing revolutionary medicine was how to do much, much more with much, much less while conceptualizing much, much deeper. In a different political climate, doctors became different people. “When I started my medical career,” Dr. Julio López shared, “I thought that if a child died of hunger it was not my problem as a doctor. But now I understand that it is my problem.”
The imperative to serve the underserved assumed the role of a theory which guided the direction of medicine in Cuba. As Karl Marx realized, “theory becomes a material force when it grips the masses.” The desire of isolated physicians to provide free care to the multitude of impoverished Cubans could not change medicine-as-an-entity. Just as futile would be a government attempting to create a new medical system by decrees that were isolated from the mood of the country. But, in a country where thousands of doctors had struggled for decades to create equitable health care, a revolutionary government which reflected that awareness could unite those struggles and reshape medicine.
The consciousness of the 3000 who stayed became a material force in the production of Cuban health care. That consciousness was as much a material force as the manufacture of pharmaceuticals or the construction of hospitals.
Unanswered was whether this new medical consciousness would be powerful enough to overcome new challenges. The need for basic services was so severe that meeting it meant building physical facilities and focusing on specific illnesses and health problems. The relationship of health care institutions to communities served remained pretty much the same. The question remained: Once the delivery of services improved, would the medical field be able to conceptualize fundamental changes in the way health care was delivered?
___________________________________
Don Fitz is on the National Committee of The Green Party USA, produces Green Time in conjunction with KNLC-TV and can be reached at fitzdon@aol.com
Go to Original – telesurtv.net
DISCLAIMER: The statements, views and opinions expressed in pieces republished here are solely those of the authors and do not necessarily represent those of TMS. In accordance with title 17 U.S.C. section 107, this material is distributed without profit to those who have expressed a prior interest in receiving the included information for research and educational purposes. TMS has no affiliation whatsoever with the originator of this article nor is TMS endorsed or sponsored by the originator. “GO TO ORIGINAL” links are provided as a convenience to our readers and allow for verification of authenticity. However, as originating pages are often updated by their originating host sites, the versions posted may not match the versions our readers view when clicking the “GO TO ORIGINAL” links. This site contains copyrighted material the use of which has not always been specifically authorized by the copyright owner. We are making such material available in our efforts to advance understanding of environmental, political, human rights, economic, democracy, scientific, and social justice issues, etc. We believe this constitutes a ‘fair use’ of any such copyrighted material as provided for in section 107 of the US Copyright Law. In accordance with Title 17 U.S.C. Section 107, the material on this site is distributed without profit to those who have expressed a prior interest in receiving the included information for research and educational purposes. For more information go to: http://www.law.cornell.edu/uscode/17/107.shtml. If you wish to use copyrighted material from this site for purposes of your own that go beyond ‘fair use’, you must obtain permission from the copyright owner.
Read more
Click here to go to the current weekly digest or pick another article:
LATIN AMERICA AND THE CARIBBEAN: